 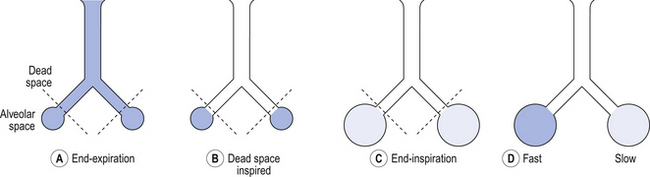
In the mainstream approach the infrared light source and sensor are placed in the primary airflow tube so that expired gas is sampled directly during expiration and the CO 2 signal is in-phase with the air-flow and pressure signals. Expired CO 2 can be obtained by sampling either mainstream or side-stream expiratory flow. Time-based capnography refers to the elimination of CO 2 over time and gives an indication of ventilation inefficiency. Capnography is the measurement of expired PCO 2. When CO 2 production and total ventilation (VE) are constant, arterial PCO 2 (partial pressure of carbon dioxide) increases in proportion to the increase in VD. Depending on the disease condition, additional mechanisms that can contribute to an elevated physiological dead space measurement include shunt, a substantial increase in overall V'A/Q' ratio, diffusion impairment, and ventilation delivered to unperfused alveolar spaces.Ventilation dead space (VD) refers to the parts of the lung and airways that do not partake in the clearance of carbon dioxide (CO 2) and indicates the inefficient portion of ventilation. For the range of physiological abnormalities associated with an increased physiological dead space measurement, increased alveolar ventilation/perfusion ratio (V'A/Q') heterogeneity has been the most important pathophysiological mechanism. Although a frequently cited explanation for an elevated dead space measurement has been the development of alveolar regions receiving no perfusion, evidence for this mechanism is lacking in both of these disease settings. An elevated physiological dead space, calculated from measurements of arterial CO2 and mixed expired CO2, has proven to be a useful clinical marker of prognosis both for patients with acute respiratory distress syndrome and for patients with severe heart failure. 
0 Comments
Leave a Reply. |
Details
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
